Peptide-drug conjugates (PDCs) are emerging as powerful tools in cancer therapy, offering new hope for patients. With the ability to precisely target cancer cells, PDCs promise fewer side effects compared to traditional treatments like chemotherapy. Researchers and pharmaceutical companies are investing in this innovative technology to tackle cancer more efficiently. By connecting potent drugs with peptides, these conjugates are designed to hone in on malignant cells, leaving healthy tissue largely untouched. This targeted approach is garnering attention globally, signaling a potential shift in how cancer might be treated in the near future.
Understanding PDCs: Components and Mechanism
What Are Peptide-Drug Conjugates?
Peptide-drug conjugates represent a sophisticated blend of pharmacology and molecular biology. At their core, PDCs are made by conjugating a cytotoxic drug to a peptide, which acts as a delivery vehicle to the tumor site. These conjugates are crafted to take advantage of the binding properties of peptides, ensuring that they deliver the drug payload directly to cancer cells.
Key Components: Peptide, Linker, Payload
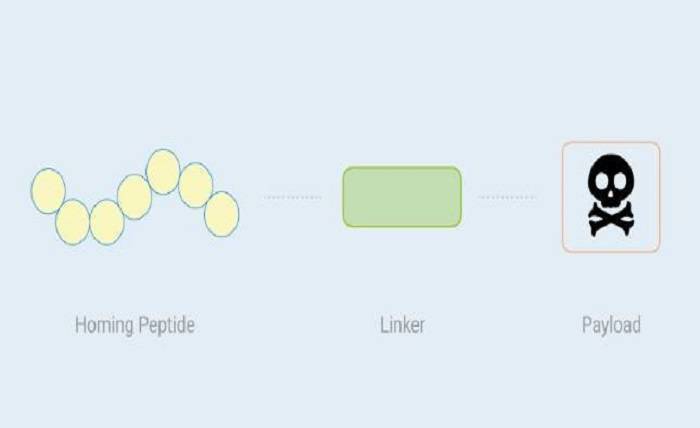
PDCs comprise three primary components: the peptide, the linker, and the payload. The peptide is a short chain of amino acids that targets and binds to specific receptors on cancer cells. The linker is an essential component, connecting the peptide to the cytotoxic drug or payload. It plays a critical role in ensuring the drug is only released at the intended location. The payload is the therapeutic agent, usually a well-studied cytotoxic drug, tasked with killing cancer cells upon release.
How PDCs Work at the Cellular Level
The mechanism of PDCs is intriguing. Once administered, the peptide seeks out and binds to specific receptors overexpressed by cancer cells. This binding triggers internalization of the PDC into the cancer cell. Inside the cell, the linker breaks down, releasing the cytotoxic agent directly where it’s needed most. This precision attack minimizes collateral damage to healthy cells, a common challenge with conventional cancer therapies.
Advantages of PDCs Over Traditional Therapies
Precision Targeting with Minimal Side Effects
Peptide-drug conjugates (PDCs) excel at precisely targeting cancer cells. By binding to specific cell receptors, they deliver toxic payloads directly to tumors. This targeted approach significantly reduces off-target damage. As a result, patients experience fewer side effects—such as hair loss or weakened immunity—commonly associated with traditional chemotherapy, making PDCs a promising tool in modern cancer therapy.
Improved Drug Stability and Bioavailability
Peptide-drug conjugates offer enhanced stability and bioavailability. Their optimized peptide-linker design keeps the drug stable in the bloodstream, ensuring it reaches cancer cells effectively. This targeted delivery allows for sustained drug release, improved therapeutic outcomes, and reduced systemic toxicity—making PDCs a powerful tool in precision oncology.
Comparison with ADCs and Chemotherapy
Compared to antibody-drug conjugates (ADCs) and conventional chemotherapy, PDCs offer several benefits. ADCs, while effective, have limitations in size and penetration. PDCs, being smaller, can penetrate tumors more effectively. Chemotherapy, though broadly used, often harms healthy tissues and leads to significant side effects, a challenge PDCs aim to overcome, offering targeted treatment with fewer drawbacks.
Clinical Progress and Market Adoption
Notable PDC Candidates in Clinical Trials
Several promising peptide-drug conjugate (PDC) candidates are advancing through clinical trials. Designed to precisely target cancer cells, these compounds demonstrate strong potential in terms of efficacy and safety. Early data highlights their ability to minimize side effects while maximizing treatment benefits. Continued research will determine their viability and long-term impact in real-world oncology settings.
Success Cases and Regulatory Outlook
Clinical trial success stories are driving regulatory approvals, as agencies increasingly recognize the promise of peptide-drug conjugates (PDCs). This growing trend reflects confidence in their targeted efficacy and reduced toxicity. As more clinical data becomes available, PDCs are expected to gain broader acceptance, reinforcing their role in advancing precision medicine and transforming cancer treatment outcomes.
Industry Trends and Pharma Investments
The pharmaceutical industry is rapidly embracing peptide-drug conjugate (PDC) technology. Companies are forming strategic partnerships to harness PDCs’ precision and effectiveness. Investment in PDC research and development continues to grow, underscoring confidence in their therapeutic potential. This momentum reflects a strong belief that PDCs will play a transformative role in the future of cancer treatment.
Challenges and Future Directions
Current Developmental Limitations
Though promising, peptide-drug conjugates face key challenges. These include complex design and synthesis, potential immune responses, and limited availability of suitable peptide-receptor targets. Addressing these obstacles is essential to enhance their effectiveness, improve safety profiles, and support wider clinical adoption in targeted cancer and disease therapies.
Strategies to Improve Efficacy and Safety
Improving PDC efficacy and safety requires innovative strategies. Scientists are developing new peptides and linkers to boost targeting precision and drug release. By fine-tuning these elements, researchers aim to create PDCs customized for specific cancers, ultimately enhancing therapeutic impact while reducing harmful side effects.
Future Potential in Personalized Medicine
Looking ahead, PDCs hold potential in personalized medicine. By tailoring peptides to individual patient profiles, treatments could become more effective and personalized. Advances in genomics and proteomics could enable precision PDC design, ushering in a new epoch of individualized oncology treatments.
Conclusion
Peptide-drug conjugates are set to revolutionize cancer treatment. With precision targeting and minimal side effects, they offer a promising alternative to traditional therapies. As clinical trials advance and pharmaceutical investments increase, PDCs could become a cornerstone of personalized cancer care, helping millions of patients globally achieve better outcomes. Further research and development will be key in overcoming current challenges, unlocking PDCs’ full potential in the fight against cancer.

