Intrathecal injections deliver medication directly into the cerebrospinal fluid (CSF), allowing precise targeting of the central nervous system (CNS). This method bypasses the blood-brain barrier, offering direct access to the spinal cord and enhancing drug effectiveness. By focusing treatment where it’s needed most, intrathecal injections play a crucial role in managing severe pain and neurological disorders. They improve therapeutic outcomes while reducing systemic side effects, ultimately enhancing the quality of life for patients requiring intensive, specialized care.
Mechanism of Intrathecal Injection
Injection Pathway and CSF Distribution
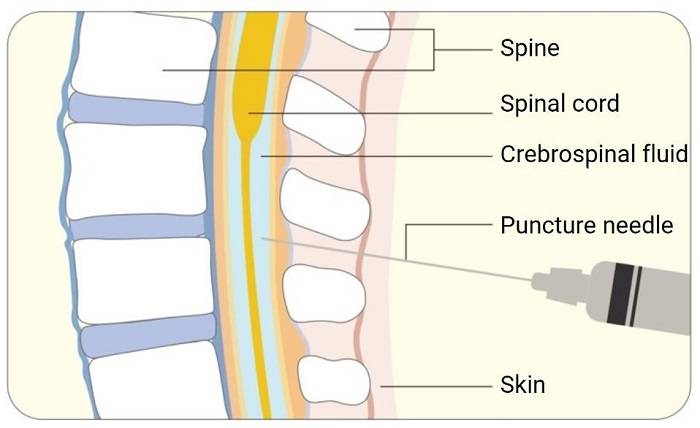
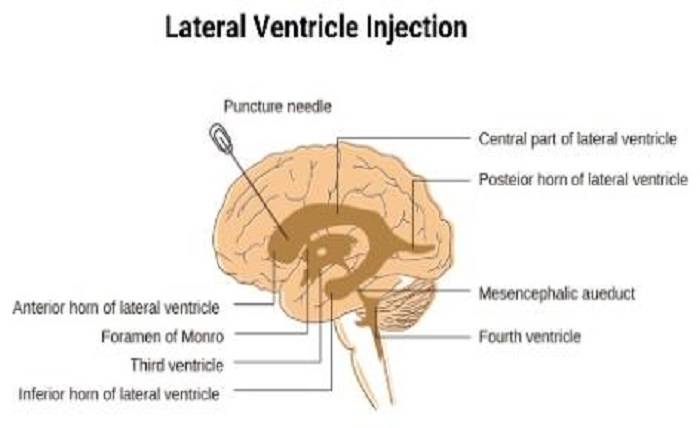
Intrathecal injections involve delivering medication into the CSF through a lumbar puncture. The drug then disperses throughout the CSF, which circulates around the brain and spinal cord. This pathway ensures direct access to the CNS, allowing for efficient distribution of therapeutic agents. The CSF acts as a medium, carrying the drugs swiftly, overcoming many conventional drug distribution limitations and providing immediate relief from symptoms associated with neurological conditions.
Role of the Spinal Cord and Meninges
The spinal cord and meninges play critical roles in intrathecal injections. The meninges, protective membranes enveloping the brain and spinal cord, include the dura mater, arachnoid mater, and pia mater. Medications injected intrathecally must traverse these layers to reach target areas. The proximity to nerve pathways allows drugs to act directly at sites of pain or dysfunction. This anatomical advantage makes intrathecal injection an effective approach for conditions that resist standard treatments.
Drug Absorption and CNS Penetration
Once administered, drugs in the CSF rapidly penetrate CNS tissues. The absorption is enhanced due to the direct contact with the brain and spinal cord, bypassing the blood-brain barrier. This facilitates higher drug concentration in the CNS compared to systemic administration routes. The direct penetration allows for reduced dosages, minimizing potential systemic side effects while maximizing the therapeutic impact on targeted neural sites.
Tools and Techniques Used
Needle Insertion and Positioning
Precise needle insertion is fundamental to successful intrathecal injection. A lumbar puncture is commonly employed, with the needle carefully positioned between the lumbar vertebrae into the subarachnoid space. This technique requires skill to avoid nerve damage and ensures accurate drug delivery into the CSF. Training and experience are essential, as they significantly impact the efficacy and safety of the procedure, reducing patient discomfort.
Intrathecal Catheters and Pumps
For continuous drug delivery, intrathecal catheters and pumps are utilized. Catheters, inserted into the intrathecal space, connect to a pump delivering a steady medication flow. These devices are programmable, allowing dosage adjustments and ensuring consistent therapeutic levels. Automated delivery enhances patient comfort and compliance, particularly in chronic conditions where long-term management is necessary.
Monitoring and Imaging Guidance
Imaging techniques like fluoroscopy or ultrasound guide intrathecal injections, ensuring precision and safety. These tools allow practitioners to visualize the needle path, confirming accurate placement within the CSF. Continuous monitoring during the procedure aids in promptly addressing potential complications. Advanced imaging techniques have improved the overall success rates of intrathecal injections significantly.
Benefits of Direct CNS Delivery
Faster Onset of Action
Intrathecal injections provide a rapid onset of action due to immediate drug access to the CNS. This speed is crucial in situations requiring prompt symptom relief, such as acute pain crises or severe spasticity. The fast action enhances patient outcomes, offering near-instantaneous alleviation of debilitating symptoms, thereby improving patient satisfaction and overall treatment effectiveness.
Lower Systemic Drug Exposure
Direct CNS delivery minimizes systemic drug exposure, significantly reducing the risk of systemic side effects. The lower systemic absorption means fewer adverse reactions, which is particularly beneficial for patients who may have contraindications to certain medications when taken systemically. This leads to a safer therapeutic profile and improved patient tolerance in long-term treatments.
Targeted Relief for Neurological Issues
Intrathecal delivery provides targeted relief for specific neurological issues, including chronic pain, spasticity, and cancer-related pain. By placing medications directly where needed, this approach maximizes therapeutic efficacy and minimizes collateral damage. Patients experience more effective symptom management, contributing to enhanced quality of life and functionality.
Use Cases and Patient Scenarios
Intrathecal Use in Chronic Pain Care
Intrathecal injections offer a lifeline for chronic pain patients unresponsive to conventional therapies. Conditions such as failed back surgery syndrome or complex regional pain syndrome benefit from this direct delivery method. Patients gain significant pain relief, reduced reliance on oral medications, and improved daily functioning, reshaping their approach to chronic pain management.
CNS Drug Delivery for Cancer and MS
Patients with cancer-related pain or multiple sclerosis (MS) encounter unique challenges requiring specialized care. Intrathecal drug delivery provides targeted relief from neuropathic pain and spasticity. For MS patients, it addresses spasticity directly, improving mobility and quality of life. In cancer care, it alleviates severe pain, helping maintain dignity and comfort throughout treatment.
Patient Selection and Medical Evaluation
Appropriate patient selection is critical for successful intrathecal therapy. A comprehensive medical evaluation ensures that candidates are suitable for this intervention, considering factors like previous treatment responses and overall health status. Careful consideration maximizes the benefits for each patient while mitigating risks, ensuring the best outcomes in highly personalized care regimens.
Conclusion
Intrathecal injection represents a powerful tool in managing complex CNS conditions. By using the intrathecal route, drugs are delivered directly to the central nervous system, resulting in faster, more effective treatments with fewer systemic side effects. Understanding the mechanisms, tools, and benefits of this approach helps medical professionals provide informed, targeted care. By harnessing these advanced techniques, healthcare providers can significantly improve outcomes and expand the therapeutic landscape for patients facing challenging neurological and chronic pain disorders.